Bloodborne Pathogen Training Course
This Frontline LMS course provides a deep understanding of bloodborne pathogens, associated risks, and how to prevent occupational exposure.
Who It’s For: Safety managers, supervisors, maintenance teams, and contractors
Time to Watch: 8–10 minutes
Summary
Bloodborne pathogens are microorganisms present in human blood that can cause serious disease. These include viruses such as Hepatitis B (HBV), Hepatitis C (HCV), and Human Immunodeficiency Virus (HIV). All these viruses pose significant workplace safety risks when workers encounter blood or other potentially infectious materials (OPIM). While healthcare environments are the highest risk for this type of exposure, others like manufacturing, utilities, emergency response, and facilities management have similar risks.
A strong bloodborne pathogens program goes beyond basic awareness training. It includes hazard identification, standardized work practices, proper use of personal protective equipment, and clear procedures for exposure response and follow-up care. Companies that combine these practices with training and documentation systems can reduce risk, improve compliance, and create a more proactive safety culture.
Key Takeaways
- Bloodborne pathogens transmit through exposure to infected blood or bodily fluids entering the body.
- HBV and HIV are the primary focus of OSHA’s Bloodborne Pathogens Standard.
- Exposure occurs through broken skin, mucous membranes, or sharps injuries.
- Universal precautions require treating all blood and bodily fluids as potentially infectious.
- PPE, hygiene, and safe work practices form the foundation of exposure prevention.
- Employers must provide training, vaccinations, and documented exposure response procedures.
- Digital systems improve training consistency, tracking, and audit readiness.
What are Bloodborne Pathogens?
Bloodborne pathogens are disease-causing microorganisms carried in the bloodstream. Unlike airborne or contact-based pathogens, these organisms require a specific route of entry into the body to cause infection. This distinction makes them both highly dangerous and highly preventable when proper controls are in place.
There are four primary categories of pathogens
- Parasites
- Bacteria
- Fungi
- Viruses
Among these, viruses are the biggest concern in the workplace because they can survive within host cells and replicate over time. This means that workers might not show symptoms until long after exposure. For many teams, a virus can spread quickly without warning if workers don’t have symptoms for a while.
Bloodborne pathogens are unique because you might not detect them in individuals who show no visible symptoms. This creates a situation where workers can’t rely on visual cues to determine risk. Instead, they must always follow standardized precautions, regardless of the perceived condition of the source individual.
Free Training Quiz
This free quiz template covers some basic questions for your workers to answer about bloodborne pathogens.
How Do Pathogens Enter the Body?
Preventing exposure begins with understanding the routes of entry for bloodborne pathogens. In the workplace, the most critical area of concern is direct blood exposure.
Pathogens can enter through broken skin, including cuts, abrasions, burns, or even minor irritations. These openings provide a direct pathway into the bloodstream. Mucous membranes such as the eyes, nose, and mouth are a high-risk entry point, particularly during splashes or aerosolized exposure incidents.
One of the most dangerous forms of exposure involves sharps injuries. Needlesticks or punctures from contaminated objects create a direct injection pathway into the bloodstream. This significantly increases the likelihood of infection.
Understanding how pathogens enter the body is essential for frontline workers to avoid exposure. Your safety training program should put a strong emphasis on handling sharp materials and proper disposal procedures to prevent these incidents.
Training Simplified
Learn how AmSty overhauled their training program with Frontline LMS.
Workers at Risk Across Industries
Bloodborne pathogens are a risk in any workplace, although some professions have a much higher probability of exposure. Healthcare workers are the highest risk group, but here are some other fields where workers are likely to encounter bloodborne pathogens:
- Emergency responders such as paramedics, firefighters, and law enforcement
- Maintenance and custodial staff responsible for cleaning contaminated areas
- Laboratory and research personnel handling biological materials
- Manufacturing employees assigned to first aid or incident response
- Waste management and sanitation workers
In industrial environments, exposure often occurs during non-routine activities. These include responding to workplace injuries, cleaning up spills, or handling contaminated equipment. Because these situations are unpredictable, you need to prepare your workers to respond safely at any time.
Why is Hepatitis B the Primary Concern?
Hepatitis B remains one of the most significant bloodborne safety risks due to its durability and ease of transmission. The virus can survive outside the body for up to seven days in dried blood, making indirect exposure a real concern in the workplace.
Symptoms often resemble the flu in early stages, including fatigue, nausea, and loss of appetite. However, the disease can progress to more severe conditions such as liver damage or cancer. In some cases, workers may remain asymptomatic while still being infectious.
This combination of durability, delayed symptoms, and long-term health consequences makes HBV a primary focus of OSHA regulations and workplace training programs.
Vaccination is one of the most effective preventive measures for HBV. Employers must offer the vaccine to at-risk employees at no cost. Companies that actively promote vaccination often see higher participation and better overall safety outcomes.
HIV and Long-Term Health Impacts
HIV presents a different risk profile. Unlike Hepatitis B, it doesn’t survive long outside the body. However, its long latency period and severe health consequences make it a critical concern.
The virus attacks the immune system, gradually reducing the body’s ability to fight infections. Without treatment, HIV can progress to the life-threatening AIDS stage.
From a workplace perspective, the key risk factor is exposure through blood or certain bodily fluids. Because symptoms may not appear for years, workers must rely entirely on preventive measures rather than observable signs.
How Does Bloodborne Pathogen Exposure Happen?
Bloodborne pathogens spread through specific types of contact, but workplace scenarios often introduce additional complexity.
Here are some examples of how bloodborne pathogens spread:
- Providing first aid to an injured coworker
- Cleaning up blood or bodily fluids after an incident
- Handling contaminated tools or equipment
- Improper disposal of sharps or biohazard waste
- Accidental splashes to the face or eyes
These situations often occur under pressure, which increases the likelihood of mistakes. This is why safety training should emphasize both knowledge and practical application.
Universal Precautions as Standard Practice
Universal precautions eliminate uncertainty by requiring workers to treat all blood and bodily fluids as infectious. This ensures consistent behavior regardless of the situation.
In practice, this means:
- Always using appropriate PPE
- Avoiding direct contact with blood or OPIM
- Following established cleanup and disposal procedures
- Maintaining awareness during all exposure-prone tasks
Companies that successfully implement universal precautions create a consistent baseline for safety. Workers no longer need to assess risk on a case-by-case basis, which reduces variability and improves outcomes.
Personal Protective Equipment and Barrier Protection
In the hierarchy of controls, PPE serves as the last line of defense against exposure. Its effectiveness depends on proper selection, use, and maintenance. As the Center for Disease Control (CDC) puts it:
“Employers should not rely on PPE alone to control hazards when other effective control options are available. PPE can be effective, but only when workers use it correctly and consistently. PPE might seem to be less expensive than other controls, but can be costly over time. This is especially true when used for multiple workers on a daily basis.”
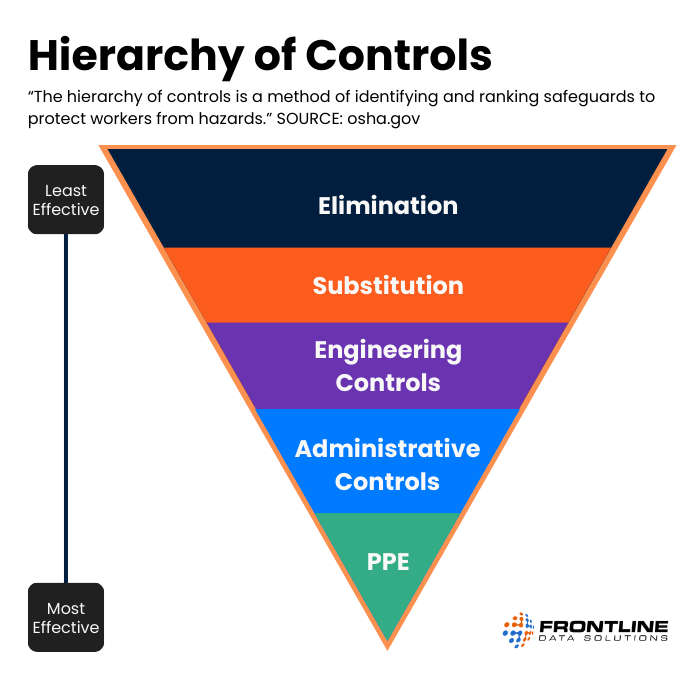
Your frontline workers should always inspect PPE before use and replace damaged equipment. To take your program a step further, ensure that workers understand when and how to use each type of equipment.
For example:
- Gloves protect against direct contact with contaminated materials
- Face shields and goggles protect against splashes
- Masks or respirators protect mucous membranes
- Protective clothing prevents contamination of personal garments
The goal is to create a physical barrier that prevents pathogens from reaching entry points.
Hygiene, Behavior, and Exposure Prevention
Hygiene practices play a critical role in preventing indirect transmission. Handwashing remains one of the most effective controls, particularly after workers take their PPE off or handle contaminated materials.
Equally important to hygiene is encouraging safe behaviors. For example, workers should avoid activities that increase the risk of ingestion or contact with bloodborne pathogens. But managers can’t spend their time micromanaging how workers go throughout their day.
Your best defense against unsafe behaviors is training, but more specifically, training that explains the why behind recommended practices. A good example is explaining to your team why they can’t eat or drink in contaminated areas. These practices may seem simple, but they require consistent reinforcement through training and supervision.
Decontamination and Environmental Controls
The decontamination process gets rid of pathogens after an exposure event. Teams should disinfect PPE, equipment, and tools that come into contact with pathogens, using solutions like diluted bleach to sanitize everything properly.
This includes:
- Cleaning all affected surfaces immediately
- Using proper contact times for disinfectants
- Decontaminating reusable equipment
- Ensuring cleaning tools themselves are properly sanitized
It’s important that workers wear protective PPE during this process, since they’re still vulnerable to exposure. Once they’re done disinfecting, things like sponges and mops need to be disinfected too. Any biohazards like needles and broken glass should go into designated containers.
Environmental controls reduce the likelihood of secondary exposure and protect workers who may not have been present during the initial incident.
Sharps Handling and Disposal Procedures
Sharps represent one of the highest-risk exposure sources. Proper handling procedures are essential to prevent injuries. Containers used for sharp materials should be leak-proof, puncture-resistant, closable, and clearly labeled.
Here are some safety tips for workers to follow when disposing of sharp objects that have been exposed to bloodborne pathogens:
- Never recap needles
- Dispose of sharps immediately after use
- Avoid overfilling containers
- Report improperly disposed sharps
These practices significantly reduce the risk of needlestick injuries.
Clear labeling and color coding ensure that workers can quickly identify hazards. Biohazard labels and red or orange-red containers provide visual cues that trigger appropriate precautions.
It’s important to remember that regulated waste includes materials capable of releasing infectious substances. Proper handling protects not only workers, but also downstream personnel involved in waste transport and disposal.
Watch the Full Bloodborne Pathogens Training
Exposure Response and Incident Management
An effective incident management program is essential for responding to and controlling bloodborne pathogen exposures. While training and preventive controls reduce risk, no program eliminates exposure entirely. The strength of your response process determines how well you protect employees after an incident, limit long-term health impacts, and prevent similar events from happening again.
An incident management program for bloodborne pathogen exposures goes beyond basic reporting. It creates a standardized, repeatable process that ensures every exposure is handled quickly, documented accurately, and investigated thoroughly. This consistency is critical in high-pressure situations where delays or confusion can lead to missed treatment windows or incomplete records.
At its core, an effective program focuses on three priorities: rapid response, thorough documentation, and continuous improvement.
Immediate Response and Reporting
The first moments after an exposure incident are critical. Employees must clearly understand what to do and feel confident taking immediate action without hesitation.
A strong incident management process ensures that workers:
- Stop working immediately when an exposure occurs
- Wash the affected area or flush mucous membranes as soon as possible
- Report the incident to a supervisor without delay
- Seek medical evaluation within the recommended timeframe
Managers should remove any ambiguity around reporting, so that workers never question whether an incident is “serious enough” to report. If there is potential exposure, it must be documented.
ACTIONABLE TIP: Establish a simple rule that if blood or OPIM contacts broken skin, eyes, nose, mouth, or results from a sharps injury, it’s automatically reportable. This eliminates hesitation and ensures consistency for critical incident reporting.
Standardized Incident Intake and Documentation
Once reported, the incident must be documented in a consistent and structured way. This is where many teams drop the ball. Incomplete or inconsistent documentation creates compliance risks and limits your ability to identify trends.
An effective intake process captures:
- Date, time, and location of the incident
- Description of the task being performed
- Route of exposure (e.g., sharps injury, splash, contact with broken skin)
- Type of material involved (blood or OPIM)
- PPE in use at the time of the incident
- Immediate actions taken by the employee
This level of detail isn’t just for compliance. It provides the foundation for identifying root causes and preventing future incidents.
ACTIONABLE TIP: Use corrective action software that requires all critical fields to be completed before submission. This reduces gaps and ensures consistency across teams.
Medical Evaluation and Follow-Up
A key component of incident management is ensuring that exposed employees receive timely medical evaluation and appropriate follow-up care. This includes:
- Confidential medical assessment
- Documentation of exposure details for healthcare providers
- Testing of the source individual when applicable
- Post-exposure prophylaxis if recommended
Speed matters. Delays in medical evaluation can reduce the effectiveness of preventive treatment.
ACTIONABLE TIP: Pre-identify healthcare providers or occupational health clinics and include them in your response plan. Workers and supervisors should know exactly where to go and who to contact.
Root Cause Analysis and Corrective Actions
Every exposure incident should trigger a structured incident investigation process. The goal is not just to document what happened, but to understand why it happened.
Effective investigations focus on identifying contributing factors such as:
- Gaps in training or understanding
- Improper or unavailable PPE
- Unsafe work practices
- Environmental or equipment issues
- Breakdowns in procedures or supervision
Once you identify root causes, implement corrective actions. These may include updating procedures, retraining employees, improving PPE availability, or modifying workflows.
ACTIONABLE TIP: Avoid stopping at “human error” as the root cause. Instead, ask what system failure allowed the error to occur. This leads to more meaningful improvements.
Get our free Root Cause Analysis Template to use for your team!
Tracking Trends and Identifying Risk Patterns
One of the most valuable aspects of an incident management program is its ability to reveal trends over time. Individual incidents may seem isolated, but patterns often emerge when you analyze data collectively.
Companies should regularly review incident data to identify:
- Repeated exposure types (e.g., frequent sharps injuries)
- High-risk tasks or locations
- Teams or shifts with higher incident rates
- Common PPE or compliance issues
This insight allows safety leaders to shift from reactive to proactive risk management.
ACTIONABLE TIP: Schedule monthly or quarterly reviews of exposure incidents and look for patterns rather than isolated events. Use these insights to prioritize training and process improvements.
Strengthening Accountability and Communication
An effective incident management program creates clear accountability at every level. Your frontline workers need to report incidents, so you can respond, document, and investigate them.
Communication plays a critical role in making this possible. Workers need feedback on incidents and corrective actions, so they understand how their reporting contributes to overall safety improvements.
ACTIONABLE TIP: Share anonymized incident learnings with teams. This reinforces the importance of reporting and helps prevent similar exposures.
Leveraging Digital Systems for Incident Management
Manual incident tracking often leads to delays, incomplete records, and limited visibility. Digital incident management systems streamline the entire process by:
- Standardizing reporting workflows
- Ensuring required fields are completed
- Providing real-time visibility into incidents
- Automating notifications and follow-ups
- Centralizing documentation for audits
These systems also make it easier to connect incident data with training and inspection data, creating a more comprehensive view of risk.
ACTIONABLE TIP: Integrate your incident management system with training records to identify whether exposure incidents correlate with training gaps or expired certifications.
Building a Proactive Exposure Response Program
The most effective incident management programs do more than respond to exposures—they prevent them. By combining fast response, structured documentation, and ongoing analysis, organizations can continuously improve their processes.
Managers play a key role in this effort. By reinforcing reporting expectations, ensuring thorough investigations, and acting on insights, they create an environment where exposure risks are actively managed rather than passively accepted.
A strong incident management program ultimately transforms exposure incidents into opportunities for improvement. Instead of isolated events, they become data points that drive better decisions, safer processes, and stronger protection for workers.
Building a Comprehensive Bloodborne Pathogens Program
An effective program integrates training, procedures, equipment, and documentation into a single system. Each component reinforces the others, creating multiple layers of protection.
Companies that take this approach move beyond reactive compliance and toward proactive risk management. They identify potential issues early, address gaps in training or procedures, and continuously improve their safety performance.
Bloodborne pathogens present a serious risk, but one that you can manage with the right approach. By understanding how exposure occurs, implementing strong preventive measures, and maintaining consistent training and documentation, you’ll be able to protect workers and maintain compliance.
Long-term success depends on consistency. When you standardize processes, reinforce training, and leverage systems like learning management platforms, you can create a safer, more resilient workplace where exposure risks are controlled before they lead to incidents.
The Role of Training in Preventing Exposure
Training ensures that workers understand both the risks and the controls associated with bloodborne pathogens. However, training must be continuous, not one-time.
Effective programs include:
- Initial onboarding training
- Regular refresher courses
- Scenario-based learning
- Post-incident retraining
This ongoing approach reinforces knowledge and keeps safety top of mind.
Frequently Asked Questions About Bloodborne Pathogens
Free EHS Training Guide
Our EHS Training Audit Guide is a great resource for evaluating your current approach to safety training and finding new ways to improve!
How a Learning Management System Improves Training Documentation
Trying to manually manage safety training often creates gaps in consistency, tracking, and compliance. A learning management system like Frontline LMS helps by centralizing and standardizing the entire training process.
An LMS allows you to assign role-specific training, ensuring that employees receive content relevant to their responsibilities. This improves both engagement and retention because workers can directly apply what they learn to their daily tasks.
From a compliance standpoint, an LMS provides real-time visibility into training completion and certification status. Safety teams can quickly identify which employees are up to date and which require additional training. This eliminates the need for manual tracking and reduces the risk of missed requirements during audits.
Automation further strengthens training programs by scheduling refresher courses and sending reminders before certifications expire. This ensures continuous compliance without adding administrative burden.
Beyond tracking, modern learning management systems improve knowledge retention through interactive content such as videos, assessments, and scenario-based learning. These methods help workers better understand how to respond in real-world situations, reducing the likelihood of errors during exposure events.
Perhaps most importantly, an LMS creates a centralized record of all training activities. This documentation provides clear evidence of compliance, supports incident investigations, and helps organizations identify trends in training effectiveness. When integrated with broader safety systems, it enables a more proactive approach to risk management by linking training data with incident and inspection data.
Frontline EHS software is a great tool for managing bloodborne pathogen exposure incidents and improving training for prevention and control. Check out our products page for more information, or book a demo to see if it could be a good fit for your program!


